Motherhood: The Most Difficult Journey Yet (Part 1)
Breastfeeding.
I always knew I wanted to breastfeed. “Babies are born to be breastfed,” La Leche League tells us. Breastmilk is chock-full of nutrients and antibodies that can’t be replicated with formula. It is linked to less health problems for the baby later in life. It helps the mother bond with the baby, ward off post-partum depression, and even assists in post-partum weight loss. It is free. It is natural. Breast is best.
Breastfeeding came naturally and relatively easy to my mother, and since so many of my pregnancy symptoms had mimicked hers — in addition to the fact that I have her body type — I had figured that it would come easily to me too.
I was wrong.

The type of blissful breastfeeding experience I had hoped to achieve with my daughter (image source)
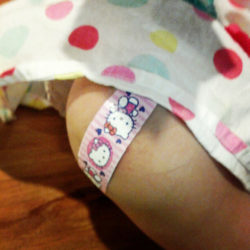
As soon as Claire returned from the nursery after receiving her first bath, the nurse who brought her in asked me if I wanted to try breastfeeding. “Of course,” I happily obliged.
There is no feeling quite like having your new baby suckle at your breast for the first time. I felt warmth and a flashing sense of euphoria for the first time since giving birth. I was doing it! I was breastfeeding!
The first “milk” that the baby receives from the breast is not actually milk. It is colostrum — a thick sticky substance that contains important antibodies and nutrients that will aid the baby to thrive in the fragile first days of life. I had read about colostrum prior to giving birth, but what I didn’t know was how little there would be of it.
Lesson #1: Colostrum is enough for the first few days.
We kept Claire in my room for the first night, and I took her to my breasts whenever she woke up and cried. Each time, she would find my nipple without a problem and latch on, sucking vigorously for a couple of minutes…then stop and turn away and cry.
I would try to guide her to my breast again, sometimes even forcing my nipple into her mouth. And the same thing would happen over and over again: she would suck for a minute or two, then stop and cry.
I tried massaging my breasts and squeezing my nipples to see if anything was actually coming out — and it was! Except…was that really colostrum? The liquid seemed thin and watery…a far cry from the thick, yellowish substance I had read about.
I reminded myself that every woman is different, and so every breastmilk/colostrum must be different too.
Later, I was to learn that colostrum, no matter how little you produce, is enough for most babies. Newborns’ stomachs are so tiny and the nutrients that colostrum provide so vast that even if your baby loses weight in the first few days after birth, he/she will not be in grave danger.
In other words, I should have trusted that my body will provide what the baby needs.
Lesson #2: Be weary of the “second day freak-out.”
I kept trying to breastfeed Claire for the remainder of that first restless night and through the next day.
But by the end of the second day, I became exhausted at my feeble attempts to provide nutrition for my newborn baby and it was clear that Claire was not happy. In-between each “feeding” (if you can even call it that), she would scream her lungs out while waving her head side to side, her mouth agape in search of satisfactory sustenance.
“She is hungry,” my mother observed.
DON’T YOU THINK I KNOW THAT?!! I wanted to shout at her.
It would be a full week later before I was to read on a parenting board of the “second day freak-out,” where a newborn suddenly realizes, “S#&T! I’m really stuck out here! I’m not going back to the warm and comfy womb!” and proceeds to cry, cry, and cry some more. Refusing to nurse properly and being especially restless and unhappy are all common symptoms of the second day freak-out.
As a mother, I needed to be patient (as hard as it may be) and just suck it up, continuing to offer my breast despite the baby’s refusal and/or protests. But I was not aware of the second day freak-out at the time, and I gave in…
Lesson #3: We should not have supplemented with formula.
After enduring what seemed like countless hours of crying (and having my heart broken over and over again…I was actually feeling physical pain over my heart), I buzzed for a nurse and asked what I should do. “Should I…give her some formula?” I asked.
“If she continues to look hungry and unsatisfied, you can go ahead,” the nurse replied.
We snapped open a single-use bottle of Similac Advance and offered it to Claire. She looked bewildered at first, but began sucking away happily. She finished more than an ounce in that one sitting! And after she was done, she burped and looked happy for the first time in over a day.
She fell asleep soon after, and stayed asleep for almost three hours — the longest stretch that she had slept since being born.
When Claire woke up from her nap, I tried breastfeeding her again. I was dismayed to find the same results: sucking for a minute or two, then stop and cry. Her latch was fine and I could not find any other source of a problem aside from the fact that I seemed to have an overly hungry baby who seemed to be a lazy and impatient suckler.
On that second night, both J and I were so tired and exhausted that we decided to keep the baby in the nursery overnight. We knew that she would be fed formula but we didn’t care. I was still gushing blood, my nipples were starting to become sore and painful, I was overly swollen from 12 hours of IV and 5 hours of pitocin, and I could barely stand up by myself, let alone take care of a newborn through another full sleepless night.
The damage had been done.
To be continued…
Read the rest of the series:
Motherhood: The Most Difficult Journey Yet (Part 3)
Motherhood: The Most Difficult Journey Yet (Part 4)
Motherhood: The Most Difficult Journey Yet (Part 5)




 I like books, gadgets, spicy food, and art. I dislike shopping, hot weather, and the laws of entropy. Although I am a self-proclaimed computer nerd, I still have a love for handbags and makeup... and I am always teetering on high heels. To learn more about me, visit the
I like books, gadgets, spicy food, and art. I dislike shopping, hot weather, and the laws of entropy. Although I am a self-proclaimed computer nerd, I still have a love for handbags and makeup... and I am always teetering on high heels. To learn more about me, visit the 


I am not a mom. Thanks for going there first and sharing. Hang in there.
I.am.taking.serious.notes. Thanks for sharing this very personal trial. Your honest and clarity are much appreciated. As Rhey said, Hang in there.
Thank you so much for sharing your experiences.
🙁 I hope "The damage had been done. To be continued…" has a happy ending and a great outcome :(((((
I love that you are so honest. Thank you for sharing.
Hi. I've been reading your blog for a while now but this is my first comment. I have felt the urge to comment previously on other posts since I feel like we share some common views but I just never did for whatever reason. Anyway, I feel compelled to comment because I know exactly what you are going through. This is just my personal experience and maybe it'll help, maybe not.
I gave birth to my son November 2009, he's 11 months now. The first couple days at the hospital were very stressful for me (amazing and wondrous at the same time of course) but also super stressful because I really wanted to breastfeed and was anxious about it – even during my pregnancy. My son came out of the womb starving (he was over 9 lbs.) and I freaked out because I wasn't producing enough at the time to feed him. I had no choice but to give him formula at the hospital. However, I made sure that we (my husband and I and the hospital staff) cup fed him so that he wouldn't get used to the nipples on the bottle. I know that there are a lot of conflicting views about nipple confusion etc. but if you're dead set on directly feeding from the breast, try the cup method. My son got used to the nipples on the bottles very quickly and it kind of caused me to give up on direct feeding. Also, my nipples were sore and torn and I just didn't have the patience or pain tolerance to stick it out especially since he loved the bottle nipples so much. Eventually, I ended up getting a nipple guard to feed him on the breast (which to him was similar enough to a bottle nipple) and then after a few months, I exclusively pumped. My son is 11-months now and I have provided breast milk for him exclusively (with the exception of the first week or two after delivery).
Also, do yourself a favor and start pumping now in addition to whatever else you're doing. Once the hospital brought me the pump and I realized that if feeding directly from the breast doesn't work, I could still feed him, my anxiety eased. The pump is awesome!
All that being said, there’s nothing like having your child feed directly from you and I encourage you to continue using your natural mama instincts to do what’s best for your child; however, just know that there are tons of options available to you.
Congrats!
First off, and most importantly: CONGRATULATIONS and HOORAY for you for two things:
– Breastfeeding :o)
and
– Blogging about it for the world to see! Exposure is the best way to encourage more to do so!
Now.
I remember when I started breastfeeding..that was over NINE years ago. Two kids later (three in total) and LOTS of research and I'm still breastfeeding my third…I do consider myself something of an expert. First, I want to tell you how sorry I am to hear about the formula – I have been horrified since my first at the way hospitals and doctors handle the breast vs. formula "debate" (especially when there should be no debate).
I just want to tell you to plow through this. The key to nursing is in the positioning. Do you have a Boppy or other nursing pillow? It helps. Look at pictures, diagrams, videos, whatever you can…it. is. all. in. the. positioning. Before I learned that, I spent six weeks in pain, crying through many many feedings, often crying right along with my son when he was hungry but would not eat. I persevered and happily nursed him until he was over two years old. To this day, he is one of the healthiest children I know, and I attribute it to the breastfeeding.
Try http://www.breastfeeding.com (especially the forums, but they have TONS of great resources there) for assistance – they got me where I am today.
Sorry for the looooooong comment – it's a passion of mine and I really hope to see you succeed!
GOOD FOR YOU!
After reading your post, I thought I would share my experience about breastfeeding.
I had my baby just one month ago. Because I was recovering from my c-section, I was unable to breastfeed for the first two days. I met with a lactaction consultant every day while I was in the hospital, and she saw how guilty I felt for not breastfeeding my baby from the very start. She told me that although it is true that breastmilk is better for baby than formula, if you can't feed the baby after a a certain amount of time, formula is certainly better than starving the baby!
Per the hospital, I kept a log of everything I fed the baby, including all attempts (successful and unsuccessful) of breastfeeding, amounts of formula, and amounts of EBM (expressed breastmilk). Looking back at my log, I saw that my baby was pretty much drinking formula the first two days (the days when I was still recovering), and started on EBM the third day. By the fourth day, when we were discharged from the hospital, the baby was breastfeeding exclusively, and has been ever since.
I'll never forget how supportive the lactation consultant was about the formula situation. I think there is too much pressure put on mothers to breastfeed that sometimes we forget there are instances where we need formula as a backup. It is not the end of the world if your baby was fed a little formula if you weren't able to breastfeed at that point in time. The thing is to get past it, and start instilling breastfeeding habits into your little one if your health now permits it.
Don't give up! The exact same thing happened to me. Don't beat yourself up or get discouraged. It took me about a month to feel comfortable breastfeeding. That was while dealing with sleep deprivation, not being able to sit due too many stiches to count, and horrible hemroids. It will get easier and you'll be a pro in no time.
A friend gave me Lansinol lanolin. It was a life saver. I now buy it for all of my friends with new breastfeeding babies.
So sorry to hear of the challenges you have been facing since Claire's birth. I am not a mom myself (maybe someday) but I watched my younger sister go through a similarly rough time with her first child. Instead of being helpful and supportive, her lactation consultant reduced her to tears on multiple occasions, guilt-tripping her heavily and not offering any workable options to help her and her baby. She continually made my sister feel like she was a terrible mom because she and her baby had such a hard time trying to make the breastfeeding work, and basically told my sister flat out that she just wasn't trying hard enough…which, like for you, was definitely NOT the case. It affected her so much that she flatly refused a lactation consultant with her second baby, remembering how thoroughly awful that woman made her feel with her first baby during what was already a very difficult time!
Maybe it's not my place to say anything, since I haven't yet had a child. But it sure sounds to me like you're doing everything humanly possible, to the point of utterly wearing yourself out, dealing with such painful physical symptoms, AND having to sacrifice a lot of time that you would much rather be actually spending with your baby. You have to do what's right for you, and no one but you can really know what that is. I'm looking forward to your post about what happened after your mom came!
While we don't know each other personally, I have really enjoyed following you on your journey to motherhood, and am learning a lot along the way. (I first came to you through the geeky girl posts) Please know that I am sending lots of supportive thoughts your way!
As a NICU nurse (and a lactation specialist) let me tell you one thing….. just because you formula fed/feed isn't the end of the world, it doesn't make you a bad parent, and anyone who tell you about nipple confusion is a big fat liar! Babies are "nipple smart" they know which one comes out faster and when they're starving they want it and they want it NOW! Breast milk comes in between 3-5 days, the more you stress the less you make. Your daughter will also sense that you're stressed and that will also affect how she will breast feed. take a few deep breaths. Offer your breast each time you feed. Put a drop of milk on your breast to get her going in you need. Some babies latch on better then others, it's ok… there's nothing wrong. I always suggest to my patients mothers, try for 15 minutes, if they just fight you, then offer the bottle, then go and pump. Remember you can always pump and give your daughter breast milk with each feed. Just don't go pump crazy, and use a really high setting thinking that that will stimulate your breast to make more milk. You'll just hurt yourself and breast feeding is so going out the window because you won't want anyone or anything to come near your breast. Don't wear yourself out, try not to stress out about it. The more pressure you put on yourself thinking that you HAVE to breast feed, or think that you're a bad mother because you gave your baby formula is going to affect your milk production. AND….. YOU HAVEN'T DONE ANY DAMAGE! Stop thinking that way!
One of my good friends had a 9 1/2 pound baby, and he screamed bloody murder the first 2 days after he was born. She called me in tears because she was at a hospital in a breastfeeding only unit and they wouldn't give her formula, She was frustrated, and tired. I went to visit her as soon as she got home, took her son and gave him a bottle, gave her my whole speech on breastfeeding, stress, and changing her thinking because she thought she would be a horrible mother if she gave formula because she was brain washed to think so. She supplemented for the first 2 weeks at most, then breast fed/bottle fed breast mile for a whole 2 years!
I'm all for breast feeding, but you need to take care of yourself too. I'm sending all the positive vibes I can.